What chronic back pain actually means
If you have been asking yourself what causes chronic back pain, you are not alone. Chronic back pain usually means pain that lasts longer than 6 to 12 weeks or keeps coming back in cycles. It often starts gradually rather than from a single dramatic injury and can involve your lower back, upper back, or neck.
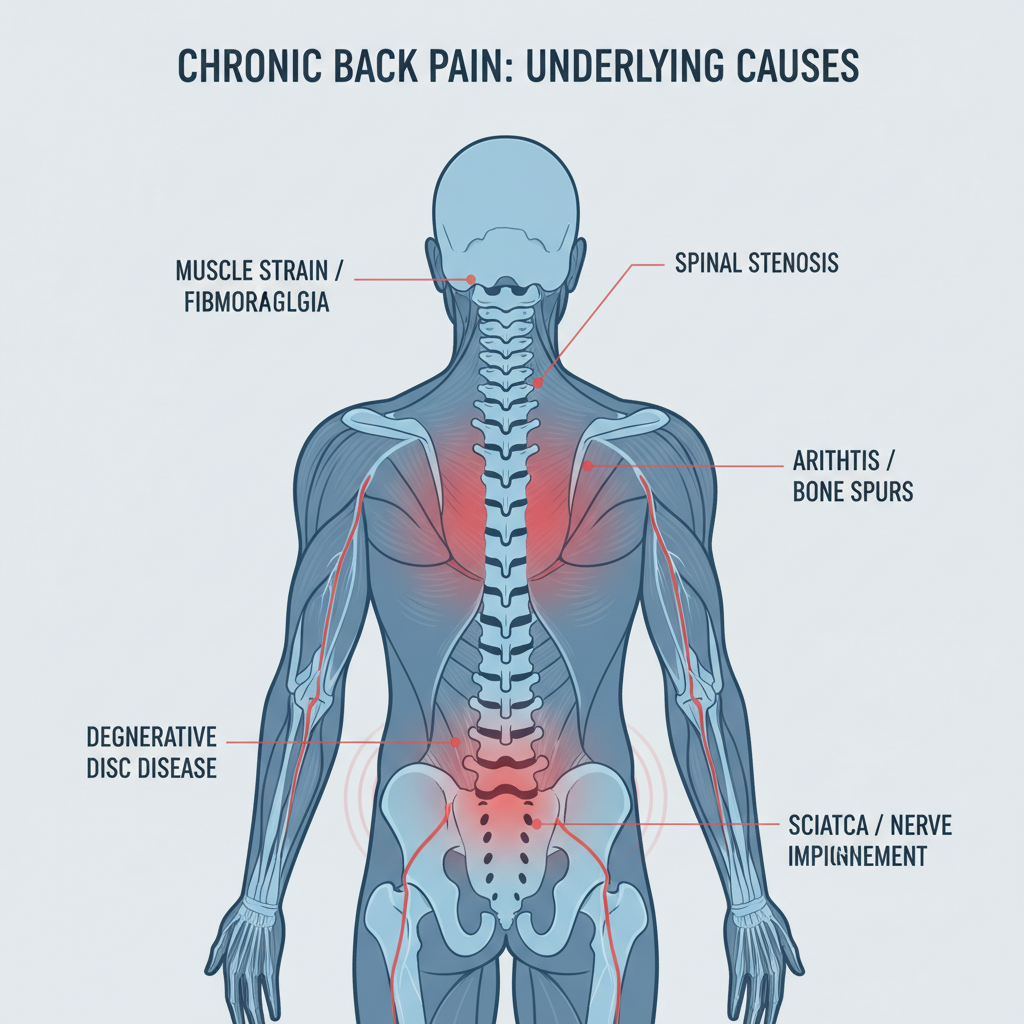
Chronic back pain is usually the result of several overlapping issues, not just one problem. Underlying conditions in your muscles, joints, discs, nerves, and even your brain and emotions can all play a role in why the pain lingers or returns. Understanding these root causes is a key step in finding the right treatment instead of only masking symptoms.
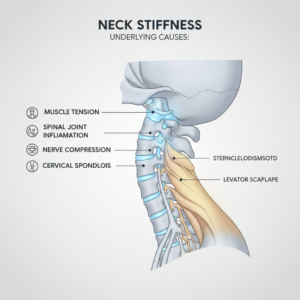
If your pain tends to move into your neck or shoulders as well, you may also want to explore why your neck hurts all the time in more detail at why does my neck hurt all the time.
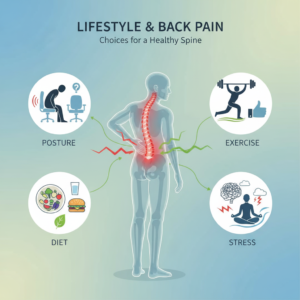
How lifestyle habits wear on your back
Daily habits and long-term lifestyle patterns are among the most common reasons back pain becomes chronic. These changes usually build up slowly until your back simply stops coping well.
Muscle deconditioning and weakness
Your spine relies on many small muscles for support. When these muscles lose strength and endurance, they cannot stabilize your back, so other structures are forced to absorb more stress.
According to HealthPartners, muscle deconditioning, often from inactivity or aging, is a frequent cause of chronic back pain because weakened muscles fail to properly support the spine and this leads to ongoing wear and tear over time [1].
You are more at risk of this type of deconditioning if you:
- Sit most of the day at work or home
- Avoid exercise because of pain or fear of hurting yourself
- Have had a previous injury that caused you to rest for a long time
- Have age-related muscle loss and have not been doing strengthening work
When your muscles are weak, everyday tasks like lifting groceries or getting out of a car can feel more demanding and can trigger recurring pain flare ups.
Poor posture and body mechanics
How you sit, stand, and move can constantly load your spine in unhealthy ways. Poor posture does not usually cause severe pain right away, but over months or years it can be a major driver of chronic back and neck pain.
Harvard Health explains that poor posture disrupts the natural curves of your spine, which increases stress on muscles, joints, and ligaments and this promotes back pain and even headaches or breathing issues [2]. When you slouch, crane your neck toward screens, or stand in a rigid, exaggerated posture, weight is no longer evenly spread across the cervical (neck), thoracic (upper), and lumbar (lower) curves.
Dr Todd Lanman notes that slouching or hunching places uneven strain on back muscles and ligaments, which leads to fatigue, tightness, and eventually chronic back pain [3]. Over time, your muscles adapt to that position, so standing up straight can actually feel unnatural and tiring.
Modern lifestyle factors that frequently contribute include prolonged sitting, poorly set up workstations, carrying heavy bags on one shoulder, high heels, and hours on a smartphone that pull your head forward into “text neck” [3]. These patterns can also compress your spinal discs and increase your risk of disc herniation and sciatica.
If you suspect posture is a major trigger for you, it can help to read more about poor posture back pain causes and specific corrections that may ease strain.
Repetitive strain and overuse
Your back is involved in nearly every movement you make. When the same tissues are stressed in the same way again and again, you can develop chronic strain injuries.
The Cleveland Clinic explains that chronic back strain often results from overuse due to prolonged, repetitive movement of the muscles and tendons that support the spine, especially in the lower back that carries much of your body weight during walking, running, and lifting [4]. Even if you never had a dramatic injury, the combination of small stresses can gradually irritate the tissues.
This can happen if you:
- Frequently lift, bend, or twist at work without proper technique
- Do physical jobs that involve pushing and pulling, such as construction or warehouse work
- Play sports like football or weightlifting that load the lower back heavily
- Have hobbies that involve repetitive motions, such as gardening or certain types of dancing
When you keep using irritated muscles or tendons without enough rest or strengthening, pain can persist and may become your “new normal.”
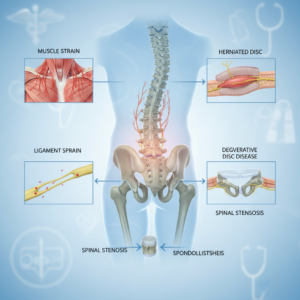
Structural problems in your spine
Sometimes chronic back pain stems from more specific changes in the discs, joints, or nerves in your spine. These structural issues can begin with a single injury or gradually appear as part of aging.
Disc herniation and nerve compression
Between each pair of vertebrae sits a disc that works as a cushion and shock absorber. When the tough outer shell of a disc weakens or tears, the soft inner material can bulge out. This is called a herniated or slipped disc.
Harvard Health describes that when a disc herniates, the displaced inner core can press on nearby spinal nerves and cause nerve-related pain, numbness, or muscle weakness [5]. In the lower back, this often leads to sciatica, which is pain that shoots from your lower back down through the buttock and leg. This pain often worsens when you cough, sneeze, or move your back suddenly [5].
Disc herniations most commonly affect the lumbar (lower back) and cervical (neck) regions, while thoracic (mid back) herniations are rare and make up less than 1 percent of cases [5].
In some cases, disc material does not just press on nerves, it also triggers a strong inflammatory response. Northwest Spine Surgery explains that when a disc slips or ruptures, it irritates nearby nerves and tissue and releases inflammatory chemicals that cause swelling and pressure on spinal nerves. This leads to sharp pain, muscle tightness, and restricted movement [6].
You might notice that even small movements like walking or bending forward cause intense pain that lasts long after the movement. This is because inflammation makes the nerves hypersensitive to mild stimuli and keeps the area irritable, which can contribute to long term pain if not addressed [6].
In rare cases, significant disc herniations can lead to serious symptoms such as muscle weakness, numbness, or loss of bowel and bladder control. Harvard Health notes that these signs suggest severe nerve compression and require urgent medical attention [5].
Degenerative changes and aging
As you age, the structures in your spine naturally change. Discs can lose height and water content, joints can become arthritic, and ligaments can stiffen. These changes are often grouped under terms like “degenerative disc disease” or “spondylosis.”
HealthPartners points out that genetic factors and the natural aging process, which reduce muscle strength and disc space, are significant contributors to chronic back pain [1]. You might notice stiffness in the morning, a sense of grinding or aching after activity, or pain that worsens gradually over years.
While you cannot stop time, you can often slow the impact of these changes through activity, core strengthening, posture work, and weight management. These habits can help your body adapt to age-related changes instead of letting them turn into constant pain.
Ligament and control system injuries
There is growing evidence that injuries to the ligaments and their embedded sensors around your spine can disrupt how your muscles and nervous system control back stability.
A hypothesis published in the European Spine Journal suggests that “subfailure” injuries to spinal ligaments, meaning they are stretched beyond their usual limit but not completely torn, can injure tiny mechanoreceptors. These sensors send signals to your nervous system about position and movement. If the signals become corrupted, muscle control around the spine becomes disorganized and can lead to abnormal loading on joints and discs over time [7].
Clinically, this may show up as:
- Delayed muscle response to sudden movements
- Trouble maintaining good posture or balance
- Muscle spasms that seem to appear easily
- Variability in how your muscles activate when you move
Over time, these altered patterns can create excessive stress and contribute to ongoing pain and degeneration. Treatment that targets neuromuscular retraining, along with managing inflammation, has shown promise in breaking this cycle for some people with chronic back and neck pain [7].
How injuries turn into long-term pain
Not all chronic back pain starts slowly. Sometimes there is a clear trigger like a fall, car accident, or lifting injury that never seems to fully resolve.
Sprains, strains, and traumatic events
A back strain involves injury to muscles or tendons, while a sprain affects ligaments. The Cleveland Clinic notes that twisting or pulling a muscle or tendon during a single improper lift can cause an acute strain, and if this is not managed properly, it can set the stage for chronic pain [4].
Sprains can result from falls, sudden twists, or impacts that push a joint out of its normal position. When ligaments are stretched or torn, joint stability can be compromised, and this may lead to lasting pain, especially if the area never fully regains strength and support [4].
HealthPartners also explains that traumatic events like car accidents or high impact falls can accelerate spinal aging and trigger chronic flare ups. Your body may adopt compensatory patterns to avoid pain, which in turn place uneven stress on other areas and maintain the problem [1].
Another issue is what happens after the initial injury. You might reduce your activity level to avoid pain. Over time, this can lead to weight gain, lower bone density, and further muscle weakening, all of which can intensify back pain and slow your recovery [4].
Repeated minor injuries
In some cases, you may never have had a major event, but small “microtraumas” have occurred repeatedly. For example, lifting slightly too heavy loads in poor form, minor car accidents, or frequent sports collisions can stretch the ligaments and soft tissues just enough to damage them without creating an obvious single injury.
The European Spine Journal hypothesis notes that single trauma or cumulative microtrauma that stretch spinal ligaments beyond their physiological limits can injure the mechanoreceptors inside them. This may lead to ongoing disruptions in muscle coordination and control that help chronic pain develop and persist [7].
The role of posture in chronic pain
Back pain and posture influence each other in both directions. Poor posture can trigger pain and chronic pain can worsen posture.
Harvard Health explains that when you slouch or tilt your head forward, the natural spinal curves are disrupted and this increases strain on muscles, joints, and ligaments, which promotes back and neck pain [2]. Over time this can even restrict your breathing or contribute to headaches.
Spine.md highlights that poor posture can compress spinal discs, raise the risk of disc herniation, and pinch nerves, which may cause radiating leg pain such as sciatica [3]. It can also create uneven pressure on spinal joints that leads to inflammation, pain, and possible long term joint degeneration.
Once you experience pain, you may unconsciously adopt “protective” positions to avoid discomfort. These can include leaning to one side, rounding your back more, or holding yourself very stiffly. Over time, these pain avoidance postures can weaken certain muscles, tighten others, and perpetuate the cycle of poor alignment and chronic discomfort [3].
If you are noticing pain higher up your spine as well, you may find it useful to read about what causes upper back pain and how posture, tension, and joint issues in that region behave.
How your mind and emotions influence pain
Chronic back pain is not only a mechanical problem. Your brain and emotional health have a major influence on how strongly you feel pain and how long it lasts.
The psychology of chronic back pain
Harvard Health notes that low back pain is one of the most common causes of disability and affects more than 80 percent of people at some point in their lives. Psychological factors such as anxiety, catastrophic thinking, and negative beliefs about your health can intensify pain by altering brain chemistry, particularly dopamine, and disrupting functions related to emotional control and attention [8].
Over time, chronic pain can cause your brain to shift more activity from pure pain sensing circuits to emotional processing circuits. This shift can increase anxiety and make it harder to modulate or “turn down” the volume of pain signals. As a result, pain can feel more overwhelming and difficult to escape [8].
The International Association for the Study of Pain (IASP) has also highlighted that depressive symptoms and common mental health disorders, including major depression and anxiety disorders, are strongly associated with chronic low back pain. These conditions increase both pain related disability and the risk that back pain will become chronic in the first place [9].
Pain and emotional distress often form a two way relationship: pain worsens your mood, and distress makes pain feel more severe. This can trap you in a loop where both keep reinforcing each other [9].
Fear, avoidance, and overactivity
How you respond to pain in your daily life also matters. The IASP describes two common behavior patterns that can worsen long term back pain: avoidance and overactivity [9].
-
Avoidance means you intentionally stop certain movements or activities because you fear pain or injury. In the short term this sometimes reduces symptoms, but over time it can lead to deconditioning, increased sensitivity, and greater disability.
-
Overactivity, or “dysfunctional persistence,” is the opposite pattern. You keep pushing through significantly painful activities and do not respect your limits. This can prevent tissues from healing and increase functional limitations.
Another key factor is pain catastrophizing, which involves exaggerated negative thoughts about pain and its consequences. High levels of catastrophizing and very low confidence in your ability to manage pain are strong risk factors for both the development and maintenance of chronic low back pain [9].
Recognizing these patterns does not mean your pain is “all in your head.” Instead, it highlights that your nervous system, emotions, and beliefs are part of the physical pain system and can either amplify or ease what you feel.
Evidence-based treatments that target causes
Once you start to understand what causes chronic back pain in your case, you can look for treatments that match those root issues instead of only masking symptoms.
Mind–body therapies and psychological treatments
Several psychological and mind–body approaches have solid evidence for helping chronic back pain.
Harvard Health notes that mindfulness based stress reduction (MBSR) has some of the strongest evidence among non drug treatments for chronic pain. MBSR can reduce pain intensity and improve emotional control, partly by increasing blood flow to the frontal lobe, which is involved in regulation and decision making [8]. However, its effectiveness can vary between individuals, particularly if there are disruptions in certain brain networks.
Cognitive behavioral therapy (CBT) helps you identify and change unhelpful thoughts and behaviors around pain. It has been shown to reduce chronic low back pain and can even help prevent acute pain from becoming chronic in some cases [8]. CBT often includes:
- Challenging catastrophic thoughts about pain
- Gradually increasing activity in a safe, structured way
- Building coping skills for flare ups and setbacks
Other approaches such as hypnosis and progressive muscle relaxation can also support pain management by lowering anxiety, tension, and overall arousal [8]. For some people, combining psychiatric medication with psychotherapy can offer added benefits, especially when depression or anxiety are prominent.
Physical therapy, strengthening, and movement
For lifestyle and mechanical causes, targeted movement based programs are often central to long term improvement. A well designed plan typically addresses:
- Core and hip strengthening to support spinal alignment
- Stretching and mobility work to ease tight muscles around the spine
- Posture training for daily tasks and work setups
- Gradual, graded exposure back to activities you have been avoiding
These strategies directly address muscle deconditioning, poor body mechanics, and the neuromuscular control issues described in the European Spine Journal hypothesis. Over time, they can help restore more normal movement patterns and reduce abnormal stress on spinal structures [7].
If your pain is closely linked to your daily habits, it can also help to review how lifestyle and movement choices affect your symptoms in more detail at how lifestyle affects back pain.
Managing inflammation and disc related pain
When inflammation from a herniated disc or irritated joints is a major driver of your symptoms, a combination of medication, physical therapy, and lifestyle changes is often recommended.
Northwest Spine Surgery notes that managing inflammation with appropriate medications, guided exercise, and adjustments in daily activities can significantly reduce discomfort from disc related back pain and in many cases can prevent the need for surgery [6].
You should seek urgent medical help if:
- Pain is severe and constant and not easing with rest
- You notice new or worsening weakness in the legs
- You experience numbness around the groin or genital area
- You lose control of bowel or bladder function
Persistent or worsening back pain beyond a few weeks, particularly if you know or suspect a herniated disc, is a signal to see a spine specialist promptly to reduce the risk of permanent nerve damage [6].
Connecting the dots for your own pain
Chronic back pain is usually the result of several factors combining over time, including lifestyle, structural issues, injuries, and psychological patterns. Two people can have similar imaging results but very different pain levels because their muscle conditioning, posture, stress, and beliefs are not the same.
To better understand your own situation, you can start by asking yourself:
- When did the pain first begin and what was happening in your life at the time
- Do certain positions, activities, or times of day make it better or worse
- Have you changed your activity level, posture, or work in ways that might stress your back
- Do you feel anxious or fearful about movement or future pain
- Have you had past injuries, accidents, or sports strains that never fully resolved
You may also find it helpful to explore why back pain keeps returning in more detail at why back pain keeps coming back, especially if your symptoms seem to settle and then flare again.
By combining what you learn about spine structures, muscle support, posture, and mind–body factors, you and your healthcare providers can move beyond the question “what causes chronic back pain” in general and instead identify what is driving yours. That understanding is often the turning point that allows you to move from short term relief to a more stable, long term improvement.