Back and neck pain can feel mysterious. Some days it is a sharp pinch when you twist, other days it is a deep, dull ache that never quite goes away. Understanding muscle tension vs spinal pain is one of the most important steps you can take if you want to know why your pain keeps coming back and what to do next.
You may not need a medical degree to sort it out, but you do need a clear picture of how your muscles and spine work together, and how lifestyle, stress, and structural issues can all play a role.
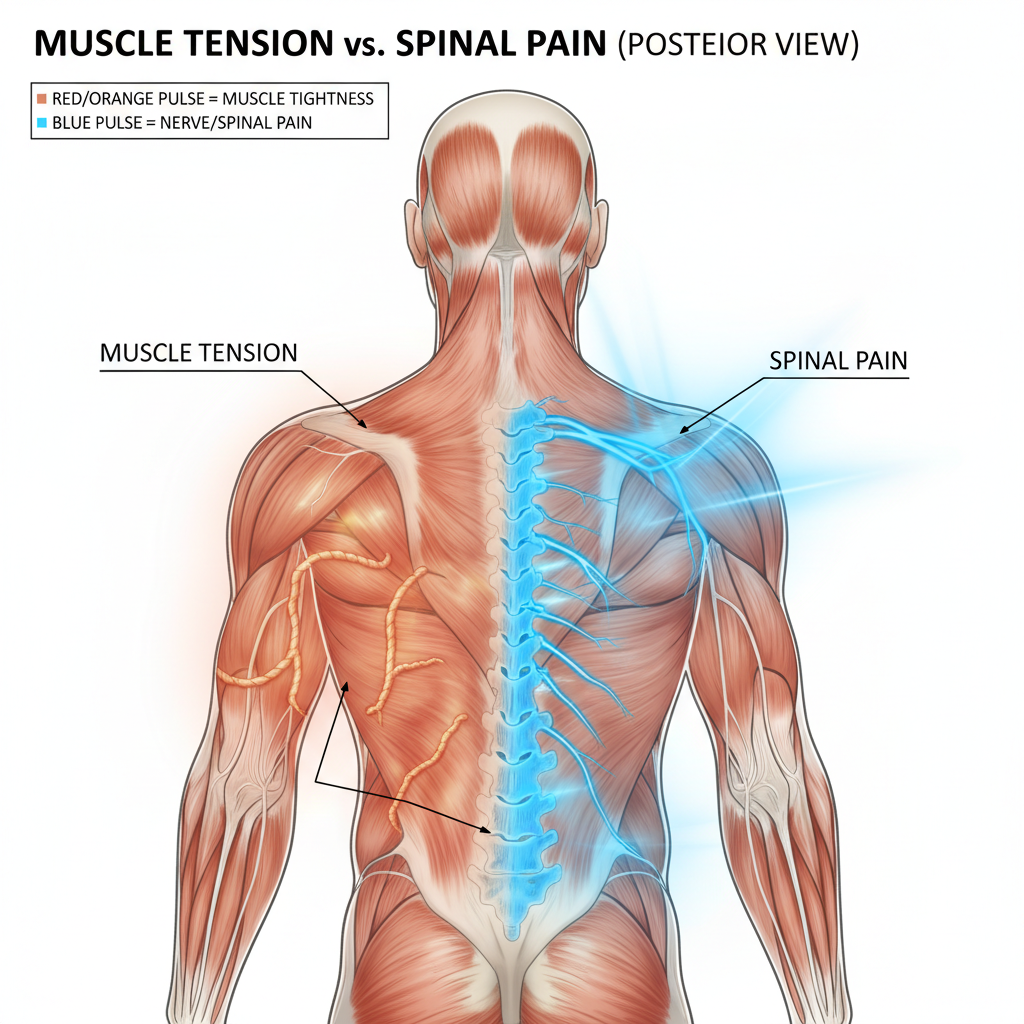
Understanding muscle tension vs spinal pain
When you talk about back or neck pain, you are usually dealing with one of two broad categories:
- Pain that mainly involves muscles and soft tissues
- Pain that mainly involves the spinal structures such as discs, joints, or nerves
You can have a mix of both, but being able to recognize which one is leading the way helps you choose better self care and know when it is time to see a specialist.
Muscle related pain is far more common than true spinal pain according to spine specialists at The PainSmith, and it often responds well to conservative treatment like rest, heat or ice, stretching, and physical therapy in a matter of days to weeks [1]. Spinal pain is less common, and although it can overlap with muscle symptoms, it is more likely to need medical evaluation and sometimes imaging or targeted interventions [1].
How muscle tension pain usually feels
Muscle tension happens when the muscles in your back or neck stay tight, overworked, or irritated for too long. This can be from poor posture, sudden overuse, stress, or a minor strain.
You are more likely dealing with muscle based pain if:
- The discomfort is focused in one main area instead of shooting far down a limb
- It feels tight, stiff, sore, or like a deep ache in the muscle itself
- Certain movements or positions clearly make it worse, such as bending, twisting, or sitting too long
- It may extend a bit into nearby areas like your buttock or hip, but not below the knee or into the hands and fingers
Experts note that muscular back pain is usually localized, may worsen with specific movements, and can cause burning, shooting, tightness, or stiffness without radiating widely into other parts of the body [1].
Muscle pain can also come in the form of back spasms. These are sudden, involuntary tightening or contractions of the muscles in your upper, middle, or lower back. Lower back spasms are especially common, and the pain can range from a small twinge to severe enough that you can hardly move [2].
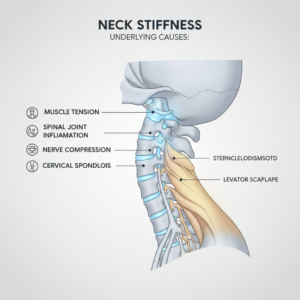
If you live with nagging neck tightness or tension headaches, you might also relate to questions like why does my neck hurt all the time or neck stiffness causes explained. In many of those cases, muscle tension plays a central role.
How true spinal pain usually feels
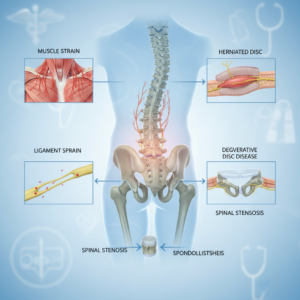
Spinal pain usually involves the joints, discs, or nerves around your vertebrae. You might hear terms like herniated disc, spinal stenosis, facet joint syndrome, arthritis, or bone spurs. All of these can irritate nerves and cause pain that behaves differently from simple muscle tension.
Spinal pain is more likely if:
- Pain radiates or travels into your legs, feet, glutes, or groin from the lower back
- Pain shoots into your shoulders, arms, or hands from the neck
- You feel numbness, tingling, or “pins and needles” along with your pain
- Weakness shows up in the affected limb, such as foot drop or trouble gripping
- The pain has been present for more than three months and is not improving with basic self care
Specialists point out that spinal pain tends to radiate to multiple areas, can include numbness or tingling, and when it becomes chronic, it needs proper medical evaluation and, in some cases, advanced imaging or procedures [1].
If you have been searching for answers on what causes chronic back pain or why back pain keeps coming back, spinal issues and long standing mechanical problems in the joints and discs may be part of your story.
Why muscle tension is so common
Muscular tightness is one of the most frequent reasons for low back pain. Often, it builds up slowly over time instead of starting with a single injury. Orthopedic specialists note that muscular tightness and limited flexibility are common causes of low back pain and that they often develop gradually due to poor posture, overuse, lack of exercise, old injuries, skeletal issues like scoliosis, and even stress [3].
A few key muscle groups often drive recurring back discomfort:
- Hip flexors and iliopsoas
- Piriformis
- Quadratus lumborum (QL)
When your hip flexors and iliopsoas muscles are tight, they can pull your lower back into an exaggerated arch, called excessive lordosis. This forward flexed, sway back posture places extra pressure on your lumbar spine and can contribute to ongoing low back pain [3].
The piriformis muscle sits deep in your buttock, attached to your sacrum. If it becomes tight or irritated, it can rub on or irritate the nearby sciatic nerve. This can cause sciatica like symptoms, such as pain, tingling, or burning that travels down the leg, a pattern sometimes labeled Piriformis Syndrome [3].
The quadratus lumborum, or QL, is a deep muscle connecting your pelvis, lumbar spine, and the 12th rib. It often steps in to compensate when your core muscles are weak, and it takes extra strain when you do a lot of lifting or twisting on one side. Over time, this can stress your lumbar vertebrae and contribute to persistent back pain [3].
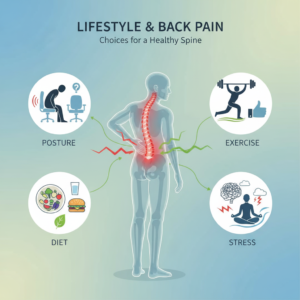
How lifestyle habits feed both types of pain
Your daily routine has more influence on muscle tension vs spinal pain than you might realize. Long hours at a desk, minimal movement, and chronic stress can slowly shape your spine and muscles into patterns that invite pain.
If you sit slumped at a computer or crane your neck toward your phone, you put extra tension on your neck and upper back. Over time, this posture can contribute to muscular pain and to structural changes that show up in conditions like disc degeneration or facet joint irritation. You can explore these patterns more deeply in topics like poor posture back pain causes and how lifestyle affects back pain.
Stress is another hidden driver. When you are under stress, your body naturally tenses muscles and increases inflammation, and your brain becomes more sensitive to pain signals. Over time, this mix can create chronic pain, stiffness, and discomfort in your back and neck [4].
Spine specialists emphasize that understanding the link between stress and back pain is key. Once you see how stress feeds muscle tension and discomfort, you can start breaking the cycle with healthier coping strategies, relaxation techniques, and regular physical activity [4]. By managing stress more effectively, you may reduce muscle tension related back pain and support better overall pain outcomes [4].
If your stress and pain are persistent and clearly linked, a consultation with an orthopedic or spine specialist can help you build a tailored plan [4].
When recurring pain points to deeper issues
When your pain keeps returning in the same way, it often signals a pattern in how you move or how your spine is coping with daily stress. Lifestyle factors such as repetitive lifting, sports, or sitting for long periods can set the stage, but underlying structural issues can keep the pain alive.
You may notice this if you find yourself reading about common causes of lower back pain, what causes upper back pain, or why neck pain gets worse over time and seeing your own experience in those descriptions.
Spinal sources of pain often involve:
- Wear and tear in the vertebrae and joints
- Disc problems such as bulges or herniations
- Narrowing of the spaces where nerves exit the spine
- Inflammatory conditions or arthritis
Over months and years, these changes can create chronic back pain that is less about a single muscle spasm and more about how mechanical stress is distributed through your spine. Experts at The PainSmith note that spinal pain can be caused by acute injuries, arthritis, vertebral wear, slipped or herniated discs, facet joint syndrome, bone spurs, osteoarthritis, or infections [1].
If your pain has lasted more than three months, radiates, or comes with numbness or weakness, it is time to treat it as a possible spinal issue rather than only a muscle strain [1].
Back spasms and what they can signal
Back spasms are often thought of as purely muscular, and many are. A sudden twist, lifting something awkwardly, or even sleeping in a bad position can trigger a painful contraction.
Back spasms are defined as sudden, involuntary tightening or contraction of muscles anywhere along your spine, with the lower back most commonly affected [2]. They can feel like anything from a mild ache or twinge to severe, incapacitating pain that makes it hard to stand up straight, and occasionally they send pain into nearby areas like your legs or hips [2].
Most simple spasms respond well to:
- Ice and heat applied in short sessions
- Gentle stretching when pain allows
- Light massage
- Gradual, consistent exercise
- Short term use of muscle relaxants if prescribed
Prolonged bed rest is no longer recommended for this kind of pain because it can weaken your muscles and actually delay recovery [2].
However, not every spasm is harmless. Sometimes, spasms can be a symptom of a more serious underlying problem such as gallstones, infections, or inflammatory spinal conditions like ankylosing spondylitis. If your spasms are accompanied by tingling, numbness, weakness, or any loss of bowel or bladder control, you should seek immediate medical attention [2].
How strength and flexibility protect your spine
It might feel counterintuitive when you are in pain, but your muscle strength plays a major role in protecting your spine from both muscle tension and spinal pain.
A large 2025 study of more than 10,000 adults in China found that those with low back pain had lower muscle strength and slower times on chair rise tests compared to those without low back pain [5]. After adjusting for factors like age, gender, education, and lifestyle, weaker grip strength and longer chair rising time were both linked to a higher risk of low back pain in adults aged 45 and older [5].
The researchers also noted that the relationship between muscle strength and low back pain risk appeared L shaped, which suggests that drops in strength have a bigger impact on pain risk when your muscles are already on the weaker side [5].
Their conclusion was clear. Interventions that improve muscle strength, such as physical therapy and strength training, have real potential to reduce low back pain and should be part of prevention strategies as we age [5].
Flexibility matters as well. Tight muscles around your spine, such as your hip flexors, piriformis, and QL, can pull your body out of alignment and increase stress on joints and discs. Regular stretching of these groups can help maintain spinal mobility and reduce strain, although stretching alone does not correct posture or deep mechanical problems. For that, guidance from a physical therapist or qualified trainer is recommended [3].
The combination of stronger muscles and better flexibility supports your spine from both sides, reducing the chance that everyday stresses will turn into recurring pain.
Safe movement when you are in pain
When your back or neck hurts, your first instinct might be to rest completely. A short rest is fine, but staying inactive for too long can weaken your muscles and prolong your recovery.
NHS guidance suggests that gradually returning to movement and strengthening after a back problem supports tissue healing and improves overall back function [6]. Some short term muscle discomfort when you start moving again is normal as your body adapts. It should settle quickly and should not make your main back pain significantly worse the next day [6].
A useful rule is to keep exercise pain in the 0 to 5 range on a 0 to 10 scale. This way you can activate and strengthen muscles without flaring spinal pain excessively [6].
Over time, you can increase strengthening exercises to about 2 sets of 15 repetitions as tolerated. This kind of consistent loading helps your muscles and tendons that support the spine grow stronger, which in turn can reduce spinal pain over the long term [6].
Gentle stretching, held for 20 to 30 seconds and done 2 to 3 times each day, can improve your range of motion and reduce muscle tension that contributes to pain in the spine [6].
If you are not sure where to start, a physical therapist can design a plan that respects both sides of the muscle tension vs spinal pain equation so that you feel safe moving forward.
When to seek medical help
You can manage many episodes of muscle based pain at home with activity changes, stretching, and short term use of over the counter pain relievers. However, certain signs mean you should get medical advice rather than pushing through.
Reach out to a professional promptly if you notice:
- Pain that radiates into your legs, feet, arms, or hands
- Numbness, tingling, or weakness in any limb
- Loss of bowel or bladder control, or trouble starting or stopping urination
- Pain after a serious fall or accident
- Unexplained weight loss, fever, or night sweats along with back pain
- Pain that is steadily getting worse or not improving after a few weeks of basic care
Back pain is extremely common, affecting up to 80 percent of people in the United States at some point in their lives, and back spasms are a frequent way that this pain shows up [2]. The good news is that with the right information and support, you can usually identify whether muscle tension or spinal issues are at the core of your symptoms.
Putting it all together for your pain
Understanding muscle tension vs spinal pain gives you a clearer map of what is happening in your body. Muscle based pain tends to be localized, closely tied to movement or posture, and often improves with rest, stretching, and strength work. Spinal pain is more likely to radiate, cause numbness or weakness, and persist beyond a few weeks, especially if underlying structural changes are present.
Your lifestyle, posture, and stress levels can influence both types of pain. When you address those root causes, build strength and flexibility, and know when to seek medical input, you put yourself in a much better position to break the cycle of recurring back and neck pain.
If you are dealing with persistent symptoms, use what you have learned here as a starting point for a more focused conversation with your health care provider. Together, you can decide whether your pain is more muscular, more spinal, or a mix of both, and what steps will move you toward lasting relief.