Neck pain that keeps getting worse over time is not just “getting older.” When you understand why neck pain gets worse over time, you can start making targeted changes that protect your spine, calm irritated nerves, and break the cycle of recurring pain.
In this guide, you will look at what is really happening in your neck, how lifestyle and aging interact, warning signs you should never ignore, and what you can do right now to stop the progression.
How your neck works and why it is vulnerable
Your neck, or cervical spine, carries a heavy load. It supports your head, which weighs about 10 pounds, all day long while also allowing you to turn, bend, and look up and down. This constant work makes the neck one of the most vulnerable regions of your spine.
The neck is made up of vertebrae, discs that cushion between them, small joints called facet joints, ligaments, and layers of muscles. Many nerves run through this compact space on their way from your spinal cord to your shoulders, arms, and hands. Because so many sensitive structures are packed into a small area, even a minor problem can create significant pain or stiffness, and that discomfort can spread into your head, upper back, or arms [1].
This complex anatomy is one reason neck pain often feels like it is “spreading” or getting worse, even if the original injury was small.
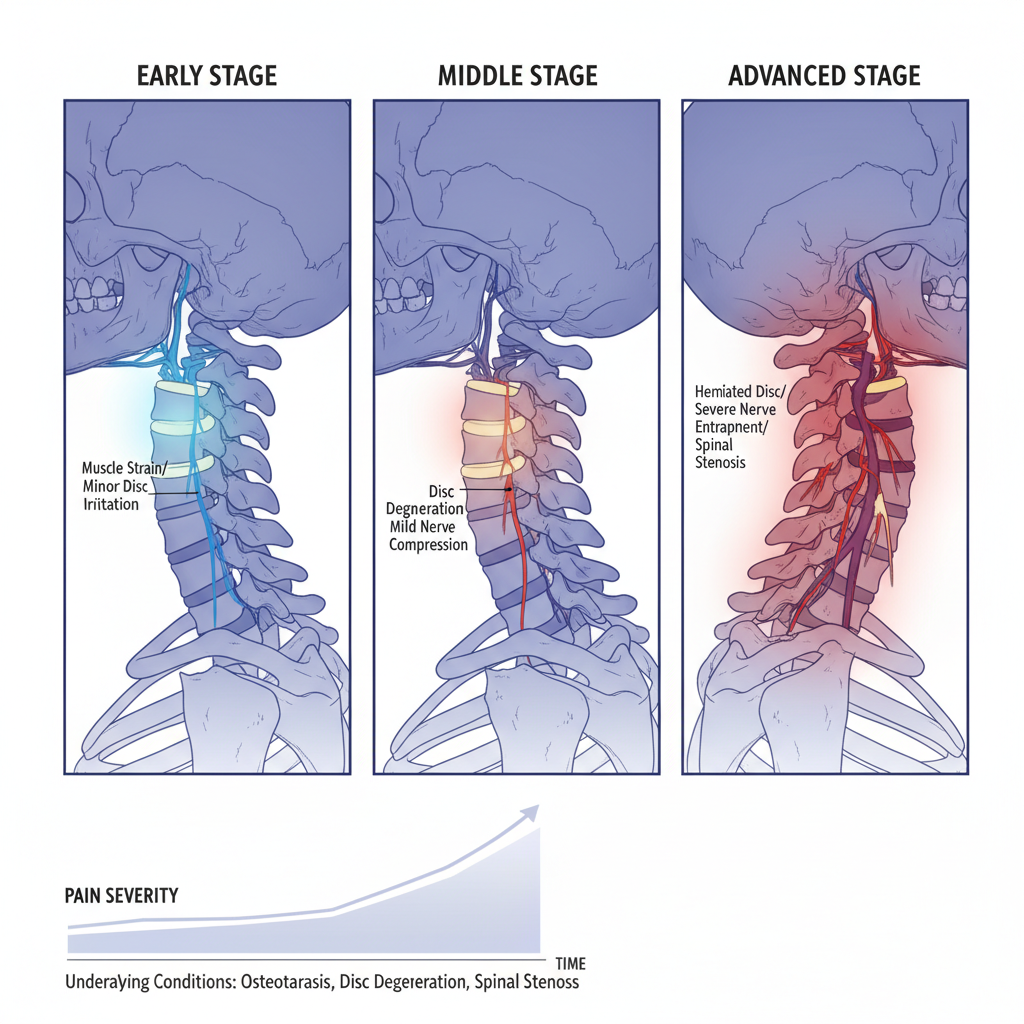
Why neck pain gets worse over time
Neck pain tends to worsen when the forces on your neck repeatedly exceed what the tissues can tolerate. Instead of fully healing, muscles, discs, and joints are stressed again and again. That repeated strain leads to gradual wear, inflammation, and eventually structural change.
Several overlapping factors usually drive this progression:
- Daily strain from holding up your head, especially with poor posture
- Degenerative changes in discs and joints as you age
- Ongoing muscle tension from stress and guarding
- Incomplete healing after injury
- Lifestyle factors like smoking, excess weight, and inactivity
Over months or years, this combination can turn occasional neck twinges into pain that lingers most days, comes back quickly after flare ups, or spreads into your shoulders and upper back. If you find yourself thinking, “why does my neck hurt all the time,” you are already seeing the cumulative effect of these forces, and you may want to read more at why does my neck hurt all the time.
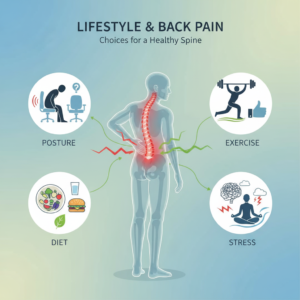
Everyday lifestyle habits that accelerate neck pain
Your daily habits often do more to shape your neck pain than any single injury. Certain patterns quietly overload the neck until symptoms become difficult to ignore.
Poor posture and “tech neck”
When you spend long hours hunched over a laptop or phone, your head drifts forward relative to your shoulders. This posture can more than double the effective load on your neck muscles and joints. Over time, that extra demand causes fatigue, tightness, and eventually pain.
Poor posture has become one of the most important reasons neck pain keeps getting worse, especially with increased screen time and work from home setups [1]. If you tend to notice neck or upper back discomfort at the end of the workday, posture is likely playing a central role. You can learn more about how this same pattern affects the rest of your spine at poor posture back pain causes.
Prolonged sitting and office work
Being an office worker is now recognized as a risk factor for chronic neck pain. Long stretches in one position increase mechanical stress on your cervical discs, especially when your neck is flexed or rotated for many hours [2].
If you sit most of the day, have few breaks, or work at a workstation that is not adjusted to you, your neck rarely gets a chance to reset. The result is gradual disc wear, stiffness, and more frequent flare ups.
Stress, muscle tension, and guarding
High stress levels can show up as constant muscle tension in your neck and shoulders. Over time, this chronic tightening reduces flexibility, alters your movement patterns, and makes it easier to re‑aggravate your symptoms.
Mental stress and poor posture together create a feedback loop: stress tightens your muscles, poor posture keeps them working harder, and pain adds even more tension. This pattern is a common reason your pain can linger beyond three months and slip into the chronic category [3].
Smoking, weight, and inactivity
Neck pain does not exist in isolation from your general health. Research on people with cervical degenerative disease found that:
- Smoking increased the risk of chronic neck pain about threefold, likely by affecting circulation, inflammation, and the health of spinal tissues [2]
- Abnormal body mass index, both obesity and underweight, was associated with worse disc degeneration and progressive neck pain
- Physical inactivity reduced blood flow and muscular support to the spine, making it easier for discs and joints to deteriorate over time
Lifestyle patterns like these are also linked to other persistent spine issues, such as what causes chronic back pain and how lifestyle affects back pain.
How aging and wear and tear change your neck
Aging alone does not doom you to severe neck pain, but age related changes can set the stage for symptoms that gradually intensify.
Degenerative disc disease in the neck
Degenerative disc disease (DDD) describes a process where spinal discs lose hydration and elasticity. In the neck, this means the cushions between your vertebrae become thinner and less able to absorb shock. As discs dry out and flatten, vertebrae move closer together and may start to move in abnormal ways.
This reduced disc height and flexibility can cause neck pain that worsens when you are upright or moving your head and improves when you lie down or recline. The altered motion and compression can also stress nearby nerves and joints, creating persistent pain or stiffness [4]. Over time, you may notice that what started as “morning stiffness” now lasts much of the day.
DDD usually develops gradually and tends to worsen with time as wear and tear continue. As the cushioning effect decreases, your neck may feel more vulnerable to everyday activities like working at a computer or driving for long periods [5].
Arthritis and bone spurs
Osteoarthritis in the neck affects the small facet joints between vertebrae. As cartilage wears down, bones can rub more directly against each other. Your body may respond by forming bone spurs, or osteophytes, around those joints and near the discs.
These bony changes can limit motion, make turning your head more painful, and sometimes press on nearby nerves. As osteophytes grow, symptoms like burning, tingling, or numbness in your shoulders, arms, or hands may appear or intensify [4]. Neck pain related to arthritis often worsens over years and may be especially noticeable with activities that involve looking up or rotating your head [6].
Spinal stenosis and nerve compression
As discs flatten and bone spurs develop, the spaces where nerves exit the spine can narrow. This narrowing, called spinal stenosis or foraminal stenosis, can squeeze nerves that travel into your arms.
Nerve compression in the neck can cause:
- Pain that radiates into the shoulder, arm, or hand
- Numbness or tingling
- Weakness or clumsiness in the hand or arm
- Electric shock sensations when bending your head forward [1]
Without treatment, this nerve irritation can become a major driver of chronic, worsening pain. Conditions like cervical spondylotic radiculopathy, where a nerve root is compressed, are strongly linked with a higher risk of ongoing neck pain compared with some other cervical conditions [2].
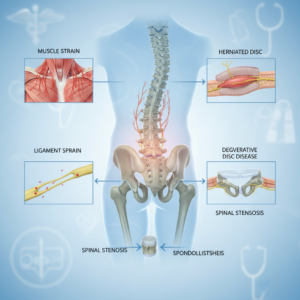
Injury, flare ups, and incomplete healing
Not all neck pain starts gradually. You might remember a specific event, like a car accident, a fall, or even sleeping in an awkward position. The problem is that after the first few days or weeks, pain often eases just enough that you resume normal activities before tissues are fully healed.
Muscle strains, ligament sprains, and even small disc injuries can leave the area weaker and more sensitive. If you do not rebuild strength and mobility through targeted exercises or physical therapy, your neck can be more easily irritated by everyday tasks. Each new flare up may last a bit longer or hurt a bit more than the last.
This pattern is similar to what many people experience with low back symptoms. Without a clear recovery plan, you may find yourself cycling through episodes that feel random, even though the underlying vulnerability is growing. You can see the same principle in why back pain keeps coming back and common causes of lower back pain.
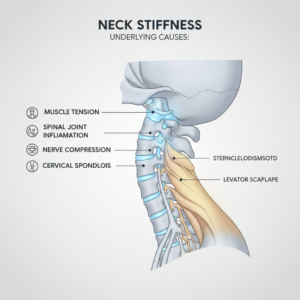
Muscle pain versus deeper spinal pain
Understanding whether your worsening neck pain is coming mainly from muscles or from deeper spinal structures can help you choose the right strategies.
Muscle based pain is often:
- Achy, tight, or burning in the neck and shoulders
- Worse after long periods in one position
- Sensitive when you press on specific muscles
- Improved with heat, massage, and gentle movement
Spine or nerve related pain is more likely to:
- Be sharp, shooting, or electric
- Radiate into the arm, hand, or upper back
- Come with numbness, tingling, or weakness
- Worsen with certain neck positions, like looking up or turning
The reality is that both often overlap. Deep problems can cause muscles to tighten and protect the area, which then creates additional soreness. For a deeper breakdown, you can explore muscle tension vs spinal pain.
Why early intervention makes such a difference
A recurring theme in current research is that untreated or poorly managed neck pain is much more likely to become chronic and severe.
If neck pain is not improving within about a week of basic self care, such as rest, gentle stretching, and over the counter anti inflammatory medication, experts recommend a clinical evaluation. Ongoing pain may be a sign of nerve compression, significant disc issues, or other problems that benefit from early treatment [1].
Delaying care allows inflammation and degeneration to progress. Over time, this can transform mild discomfort into sharp pain accompanied by muscle spasms, radiating symptoms, or loss of neck motion [7]. Once pain has lasted more than three months, it is considered chronic, and both the spine and the nervous system may have undergone changes that make pain more persistent [3].
Seeing a professional early also helps you distinguish between common mechanical causes and more serious underlying conditions. Related resources such as neck stiffness causes explained and what causes upper back pain can further expand your understanding of nearby pain patterns.
Untreated neck pain often does not simply “plateau.” It frequently progresses in severity, spreads to new areas, and becomes harder to treat over time if underlying causes are not addressed.
How to stop neck pain from getting worse
You cannot control every factor that affects your neck, but you can significantly slow or even reverse many of the forces that drive worsening pain.
Improve posture and movement
Work on small, consistent changes rather than perfect posture overnight.
- Adjust your workstation so your screen is at eye level and your shoulders can relax
- Keep your head stacked over your shoulders instead of poking forward
- Take brief movement breaks every 30 to 60 minutes to reset your muscles
- Use a supportive chair that allows your feet to rest flat on the floor
These changes reduce constant strain on your neck and help your discs and joints handle daily loads more comfortably.
Strengthen and stretch key muscles
Gentle, regular exercise is one of the most effective ways to manage degenerative disc disease and related neck pain [5]. A physical therapist can design a plan, but common elements include:
- Deep neck flexor strengthening to support the front of your neck
- Upper back and shoulder blade exercises to offload your cervical spine
- Stretching for tight chest, upper trapezius, and levator scapulae muscles
- Controlled mobility drills that restore comfortable neck rotation and bending
Strengthening creates a muscular “brace” that protects aging discs and joints, while stretching reduces the constant pull of tight tissues on sensitive structures.
Manage stress and muscle tension
Since stress is a powerful driver of persistent neck muscle tension, addressing it directly can ease pain and prevent flare ups from escalating.
You might experiment with:
- Breathing exercises or meditation
- Short walks throughout the day
- Gentle yoga or tai chi
- Brief self massage of the neck and shoulders with heat
Reducing baseline tension helps your neck respond more calmly to daily demands and reduces the risk that minor discomfort will spiral into a full flare.
Address lifestyle risk factors
Gradual steps toward healthier habits can protect your neck in the long term.
- If you smoke, consider structured support to stop, since smoking is linked with worse neck disc degeneration and higher chronic pain risk [2]
- Work toward a stable, healthy weight to limit mechanical load on your spine
- Stay as active as your symptoms allow, since movement supports disc nutrition and joint health
These same changes often help with persistent lumbar pain and broader spinal issues, which you can read more about at how lifestyle affects back pain.
Seek professional help when needed
You should seek prompt medical evaluation if you notice:
- Neck pain that does not improve after one to two weeks of self care
- Radiating pain, numbness, or tingling into your arm or hand
- Weakness, clumsiness, or dropping objects
- Electric shock sensations when you bend your head forward
- Problems with balance, walking, or bladder or bowel control
These symptoms can suggest significant nerve involvement or spinal cord pressure that should not wait.
Depending on your situation, treatment may include medication, targeted physical therapy, guided injections, or in more advanced cases, surgical options such as decompression or disc replacement. For example, cervical disc replacement aims to maintain motion at the treated level and may reduce the risk of further degeneration at nearby discs compared with traditional fusion surgery [4].
Putting it all together
Neck pain often gets worse over time because of constant mechanical strain, age related disc and joint changes, chronic muscle tension, and lifestyle factors that gradually overwhelm your spine’s ability to recover. The longer these forces act without being addressed, the more likely your pain is to become chronic and to spread beyond your neck.
You are not powerless in this process. By improving your posture, staying active, strengthening and stretching key muscles, managing stress, and addressing risk factors like smoking and prolonged sitting, you can slow or even reverse many of the changes that drive worsening pain.
If you are already living with persistent symptoms, using what you have learned about why neck pain gets worse over time can help you have a more productive conversation with your healthcare provider and make informed decisions about the next steps in your care.